This means that if the BMI association had been properly estimated by accounting for its nonlinear effects, BMI would almost certainly be a better predictor than WHR for women specifically,” she said.ĭr. “BMI was just as good as WHR at predicting all-cause mortality for women (though not for men). “I do think some of the conclusions of this new study are potentially misleading,” she told Healthline. Maya Mathur, PhD, an assistant professor of the Quantitative Sciences Unit at Stanford School of Medicine, commended the study for its strong sample size and use of Mendelian Randomization to account for genetic factors but ultimately disagreed with its conclusions. However, the suggestion that WHR is more accurate than BMI was disputed by other experts contacted by Healthline.ĭr. We didn’t find a limit where no additional benefit was seen,” Dr. “Our research shows that the lower the better. Common guidelines suggest a WHR of < 0.95 in men and < 0.80 in women. Unlike BMI, where there is a healthy range, a WHR score should be as low as possible. Paré and his team argue that WHR offers a simple, easy-to-read, accurate measurement. Whereas BMI had worse outcomes at lower ranges, then improved in the middle (healthy BMI range), before worsening again as BMI entered overweight and obesity levels. What that means in its simplest form is that every increase in WHR leads to worse health outcomes, no matter your BMI. When comparing BMI and WHR to all-cause mortality, they found that BMI followed a “J-shaped association,” whereas WHR had a direct linear association. Researchers used Mendelian Randomization, which uses genetics to help account for inherent predisposition for things like cardiovascular disease and cancer. 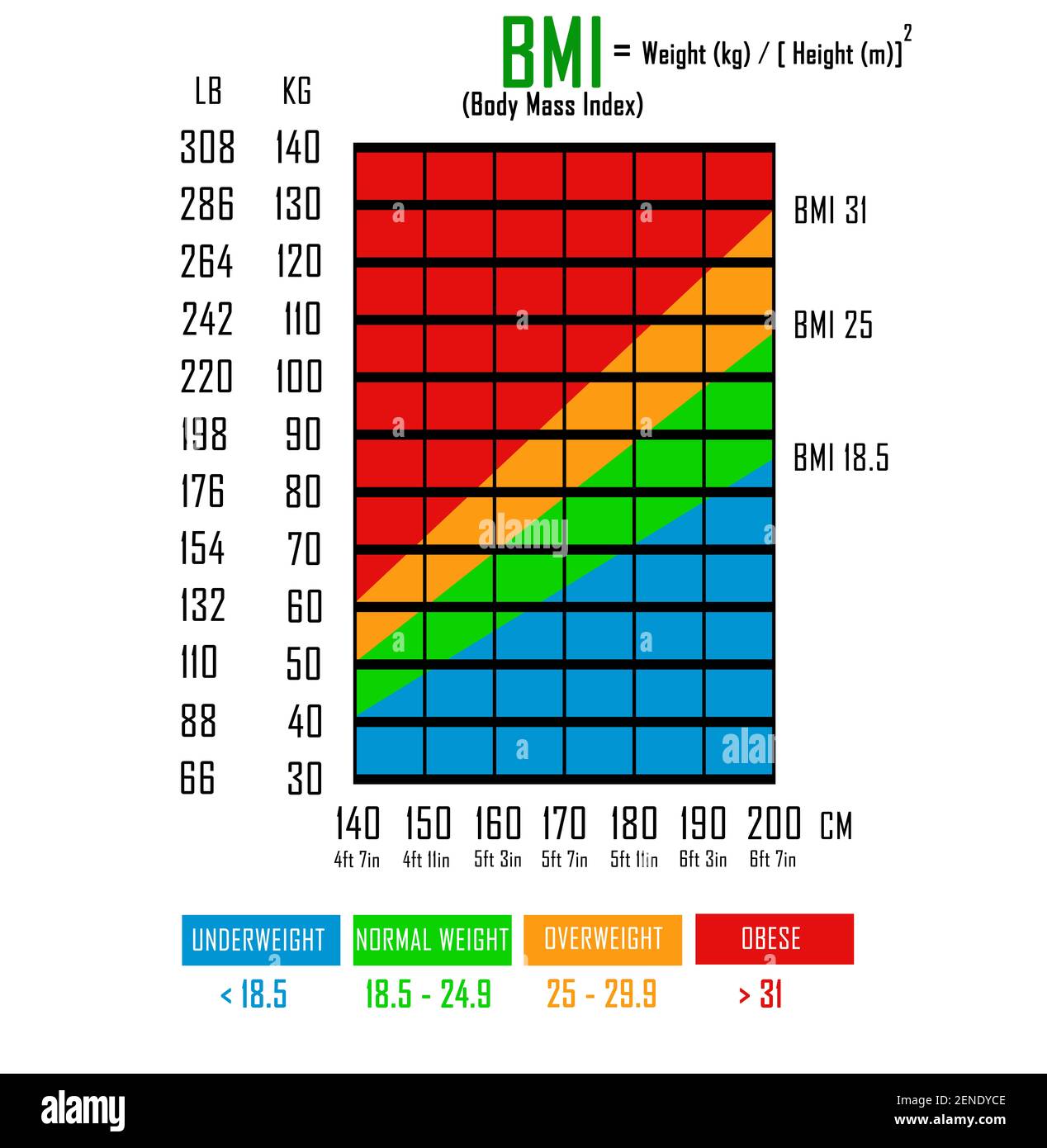
Participants included 387,672 participants in the United Kingdom with an average age of around 60 years old. “These findings support the increasing body of literature that have shown WHR to be superior to BMI, and suggest WHR should be used clinically,” he said.įor the study, Paré utilized the UK Biobank, a medical research database containing anonymous health and lifestyle information about its participants. Guillaume Paré, MD, a Professor of Medicine at McMaster University and lead author of the research, told Healthline. For this specific project, we aimed to determine what is the best way to assess adiposity,” Dr. “We are interested in understanding what are the risk factors for cardio-metabolic diseases and how best to assess them. Their conclusion: “WHR had the strongest and most consistent association with mortality irrespective of BMI.”įurthermore, the researchers say their findings have implications for the doctors’ office, too, arguing that using WHR as a primary measurement of health could lead to better outcomes than BMI alone. In a study published on September 20 in the medical journal JAMA Network Open, researchers looked at nearly 400,000 individuals to see whether BMI or waist-to-hip ratio (WHR) was a more accurate predictor of serious adverse health outcomes, including: New research suggests that waist-to-hip ratio could be a simpler, more accurate indicator of weight and general wellness than BMI. If you’ve been in for a checkup in the past year, you probably know your body mass index (BMI). 
0 Comments
Leave a Reply. |
AuthorWrite something about yourself. No need to be fancy, just an overview. ArchivesCategories |
 RSS Feed
RSS Feed
